| Key Points | Details to Remember |
|---|---|
| 🩸 | Understand that a hematoma is a collection of blood under the skin following trauma. |
| ❄️ | Apply ice within the first 48 hours to limit the extent and pain. |
| 🧷 | Compress moderately to reduce swelling without blocking circulation. |
| ⬆️ | Elevate the affected limb to facilitate lymphatic drainage and reduce inflammation. |
| ⚠️ | Consult if pain worsens, if the hematoma spreads rapidly, or if there are neurological signs. |
| 💊 | Avoid anticoagulants if possible without medical advice, and use safe analgesics. |
A bruise that swells and changes colors, a purple spot on the leg after a blow: a hematoma is common, but it often causes concern. Here, I describe step by step what you can do immediately, effective home care, useful medications, and warning signs that require consultation. We maintain a pragmatic approach: ease the pain, limit progression, and promote the natural resorption of the accumulated blood.
Sommaire
What is a hematoma and how does it evolve
A hematoma corresponds to blood that escapes from a broken vessel and lodges in the subcutaneous or deeper tissues. Depending on the depth, it will appear as a surface bruise or as a firmer mass. In the hours that follow, the area swells because blood and inflammation accumulate; then, the color changes — red, purple, green, yellow — as the body reabsorbs the blood pigments. This evolution is a good indicator of healing, but it does not exclude the need for follow-up if other symptoms appear.
Difference between hematoma and simple contusion
These two terms are often confused. Contusion refers to the trauma itself; hematoma is the result, the accumulation of blood. A contusion may occur without a visible hematoma if the affected vessels are very small. Conversely, a significant hematoma indicates more marked damage to vessels and sometimes deeper tissues.
First actions to take immediately
The first 48-hour window is crucial. The actions must reduce local bleeding and swelling without risking worsening the situation. Here is a simple method, which you may already know but which is better applied precisely.
- Ice: apply ice packs wrapped in a cloth for 10–15 minutes every 1–2 hours during the first 24–48 hours. The goal is not to freeze the skin but to reduce local blood flow and pain.
- Compression: an elastic bandage can help, but without tightening to the point of cutting off circulation. Check the temperature of the fingers or toes downstream to ensure they remain well perfused.
- Elevation: raise the limb above heart level as much as possible to promote venous return and reduce swelling.
- Relative rest: avoid intense local effort for 48–72 hours; this limits the risk of extension.
Why heat is contraindicated initially
Heat increases blood flow and can amplify subcutaneous bleeding. Wait at least 48 hours before applying a mild heat source, and only if the hematoma is not worsening.
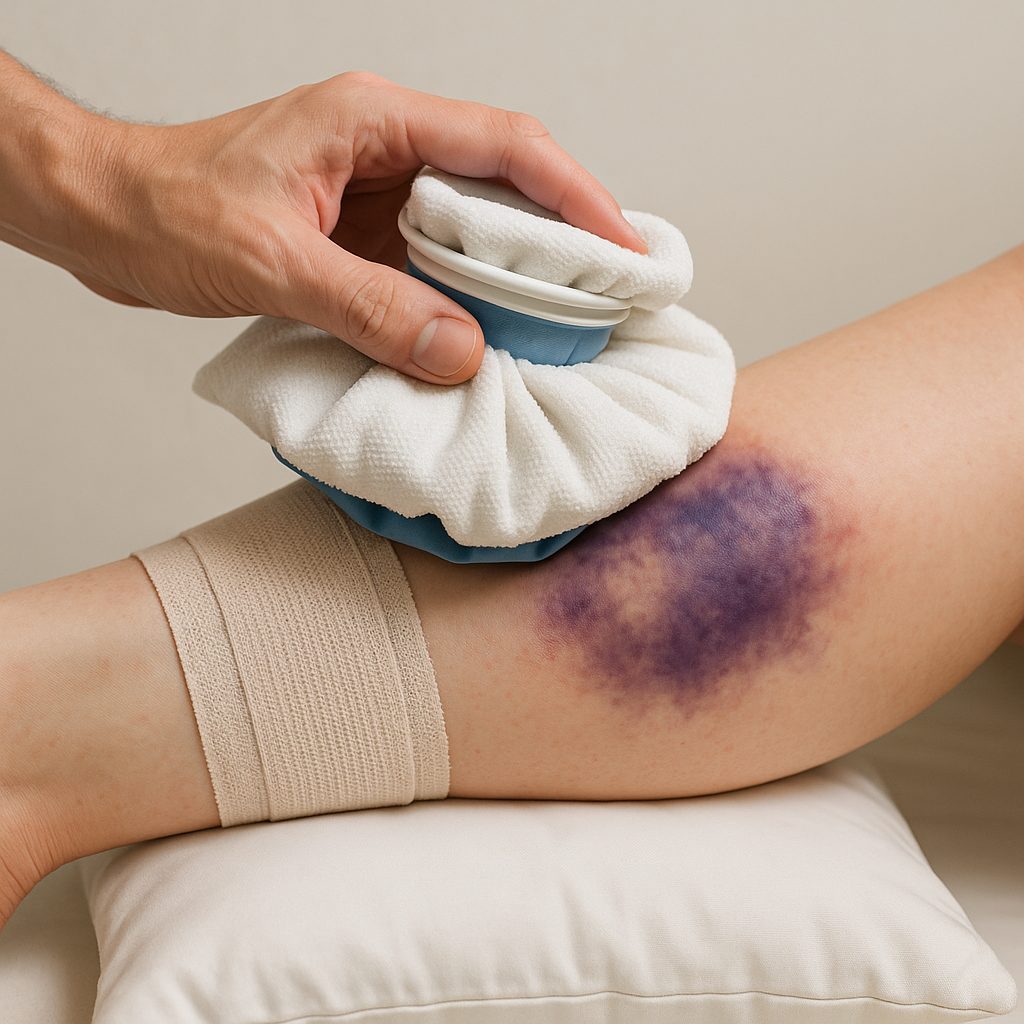
Additional treatments and effective home remedies
Beyond ice and compression, a few simple measures accelerate resorption and relieve pain. Some methods are supported by clinical experience, others by popular use; I clearly distinguish what is pragmatic from what is anecdotal.
- Active rest: gently moving the limb promotes lymphatic drainage without restarting bleeding.
- Topical hemostatic or anti-inflammatory creams: some ointments based on arnica or local heparin can help reduce bruising. Check contraindications if you are taking anticoagulants.
- Nutrition: consume vitamin C and proteins to aid tissue repair. Zinc and antioxidants also play a secondary role.
Medications: which to use, which to avoid
For pain, paracetamol remains the first choice as it does not affect coagulation. Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen relieve pain but can promote bleeding in some people; use cautiously, especially in the first days. Anticoagulants (warfarin, high-dose aspirin, new anticoagulants) require medical advice in case of a significant hematoma: sometimes therapeutic adjustment is necessary.
When to consult a professional
Most hematomas resolve within a few weeks, but some signs require prompt consultation. Monitor and act if:
- pain progressively increases or becomes unbearable;
- the hematoma spreads very quickly or forms a hard mass;
- you experience tingling, loss of mobility, paleness, or distal coldness (sign of ischemia);
- fever or significant redness: suspicion of infection;
- head trauma, near the eye, or in case of vomiting and severe headaches after a blow — go to the emergency room.
Possible examinations and interventions
The doctor may prescribe an ultrasound to estimate the extent, or a puncture if the hematoma is large, painful, and accessible. For compressive hematomas (e.g., in the thigh or calf with compartment syndrome), urgent care is necessary. Surgery is rare but indicated if the hematoma compresses vital structures or if there is active bleeding.
Special cases: head, eye, repeated hematomas
Hematomas around the head and eye require special attention. A swollen eye and a periorbital hematoma can mask a more serious injury: intense pain, visual disturbances, or limitation of eye movement require urgent ophthalmological consultation. Frequent, spontaneous, or disproportionate hematomas relative to the trauma should prompt an investigation for a coagulation disorder.
| Situation | Recommended action |
|---|---|
| Cranial hematoma after a blow | Urgent consultation + neurological monitoring. |
| Periorbital hematoma | Assess vision and mobility; ophthalmological consultation if abnormality. |
| Repeated hematomas | Perform a hemostasis workup and review medications. |
Recovery: how long, how to help the body
Complete resorption varies: small bruises in 2 weeks, deep hematomas several weeks to a few months. Light massage (after 48–72 hours and if there is no pain) stimulates lymphatic circulation and helps eliminate pigments. Physiotherapy can be useful if mobility is reduced, and compression can be prolonged if edema persists.
Prevention and long-term measures
To reduce the risk of hematomas: strengthen muscle tone around joints, protect at-risk areas during physical activities (knee pads, shin guards), and check drug interactions if you take anticoagulants or antiplatelet agents. If bruises occur without an obvious cause, seek medical evaluation.
FAQ — frequently asked questions
How long does it take for a hematoma to disappear?
It depends on its size and depth: a superficial bruise can fade in 1–2 weeks; a deep hematoma can take several weeks to a few months.Can you pierce a hematoma yourself?
No. Piercing a hematoma exposes you to infection and increased bleeding. Aspiration must be performed in a medical setting if necessary.Do arnica creams work?
They can provide local relief and reduce the appearance of bruising in some patients. They remain a complement, not a miracle treatment.What signs are alarming?
Worsening pain, rapid expansion, loss of sensation or movement, fever, or any cranial injury with neurological symptoms.
In conclusion, a hematoma is often benign but deserves careful assessment: initial measures (ice, compression, elevation) limit extent and pain, while knowledge of warning signs prevents complications. If in doubt, it is better to consult — sometimes caution shortens recovery.











