| Key Points | Details to Remember |
|---|---|
| 🔬 Definition | Understanding blood sugar levels |
| ⚖️ Normal Values | Locating your measurements by age |
| 🌡️ Measurement | Choosing a suitable device |
| 🍽️ Nutrition | Identifying low and high GI |
| 💡 Tips | Adopting natural remedies |
| 📊 Interpretation | Spotting critical thresholds |
Monitoring your blood sugar level is not just about ticking a box for people with diabetes. Every variation, even minor, can reveal insulin sensitivity or signal a need to adjust diet. Among the millions of patients monitored each year, many ignore the importance of the frequency of checks and the meaning of the numbers displayed.
Fasting, after a meal, or over months via HbA1c, these indicators map the glucose metabolism. Understanding these references is not just about memorizing numbers: it is reading your health, anticipating a trend, and potentially avoiding complications and hypoglycemia. The World Health Organization (WHO) and the American Diabetes Association (ADA) provide structured thresholds, supported by ongoing research. But at each age group, for each profile, nuances and tolerances adjust.
This guide immerses you in a blood sugar level chart, details critical thresholds, explores foods that raise or stabilize your blood sugar, and compares the latest measuring devices. Bonus: grandmother’s tips to stay on track daily.
Sommaire
Blood Sugar Level Chart According to Situations
A blood sugar level chart clarifies the key reference points to remember. Below, values are expressed in millimoles per liter (mmol/L) and milligrams per deciliter (mg/dL), to match the standards of your lab or device.
| Time of Measurement | Normal Value (mmol/L) | Normal Value (mg/dL) |
|---|---|---|
| Fasting (8–12 hours without food) | 4.0 – 5.5 | 70 – 100 |
| Postprandial (1–2 hours after meal) | < 7.8 | < 140 |
| HbA1c (2–3 month average) | < 6.0 % | — |
These thresholds provide an instantaneous view. To refine according to age and sex, this second table offers a comparison man/woman, young adult/senior. It is noted that glucose tolerance tends to narrow after 60 years, without making it an absolute rule.
| Profile | Fasting Blood Sugar | Postprandial |
|---|---|---|
| Man (30–50 years) | 4.2 – 5.5 mmol/L | < 7.8 mmol/L |
| Woman (30–50 years) | 4.0 – 5.2 mmol/L | < 7.8 mmol/L |
| Senior (60 years and older) | 4.5 – 6.0 mmol/L | < 8.0 mmol/L |
Interpretation of Values and Critical Thresholds
Beyond the numbers, it is the trend that alerts. When fasting blood sugar approaches or exceeds 5.6 mmol/L, one enters the so-called prediabetes zone, a warning signal to adjust lifestyle. A spike above 11 mmol/L after a meal may indicate glucose intolerance.
- Hypoglycemia: blood sugar < 3.9 mmol/L (70 mg/dL). Common symptoms: sweating, trembling, irresistible hunger.
- Normal zone: 4.0–5.5 mmol/L fasting and < 7.8 mmol/L after meals.
- Hyperglycemia: fasting > 7.0 mmol/L and/or postprandial > 11.1 mmol/L. Signs: increased thirst, fatigue, blurred vision.
Chronic hyperglycemia strains the pancreas and can lead to insulin resistance. Conversely, a severe hypoglycemic episode often requires rapid correction with a glucose tablet or a sugary drink.
Which Foods Influence Blood Sugar?
The glycemic index (GI) classifies carbohydrates according to absorption speed. High GI foods trigger a sudden spike, while a low GI induces a more gradual rise. This changes insulin demand and available energy.
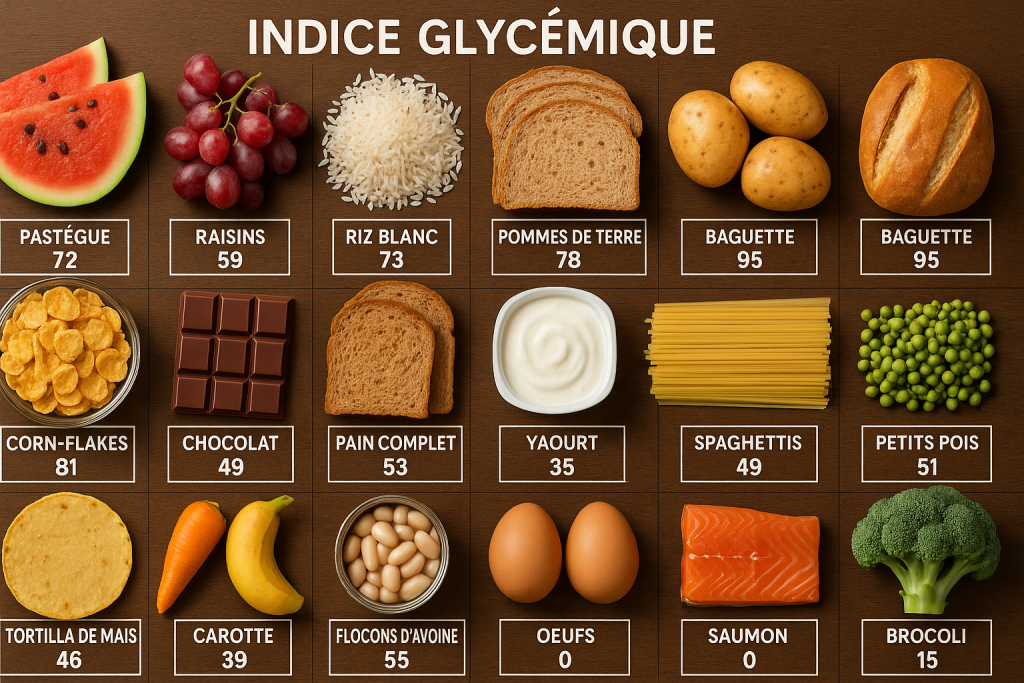

In the category of low glycemic index foods you will find legumes, most green vegetables, and some red fruits. Conversely, white bread, peeled cooked potatoes, or white rice often have a GI above 70.
- Low GI (< 55): lentils, chickpeas, split peas, tomatoes, cherries.
- Medium GI (55–69): ripe banana, basmati rice, oatmeal flakes.
- High GI (> 70): potato, white bread, chocolate bars.
Varying textures and combining fiber and protein reduces the impact on blood sugar. For example, an almond oatmeal porridge slows absorption compared to a bowl of sugary cereal.
How to Measure Your Blood Sugar?
Between finger-prick glucometers and continuous sensors, the range of devices is diversifying. The choice mainly depends on the frequency of checks, comfort, and budget.
- Blood glucose meter (glucometer): the most widespread method. After a micro-prick, a reader displays the result in a few seconds. Reliable and affordable, it can however cause discomfort during repeated tests.
- Continuous sensor: small patch stuck on the skin, it measures blood sugar continuously for 7 to 14 days. Data transmitted to a smartphone allows monitoring curves without pricks.
- Needle-free reader: emerging technologies using spectroscopy. Under validation, they could soon offer a completely painless device.
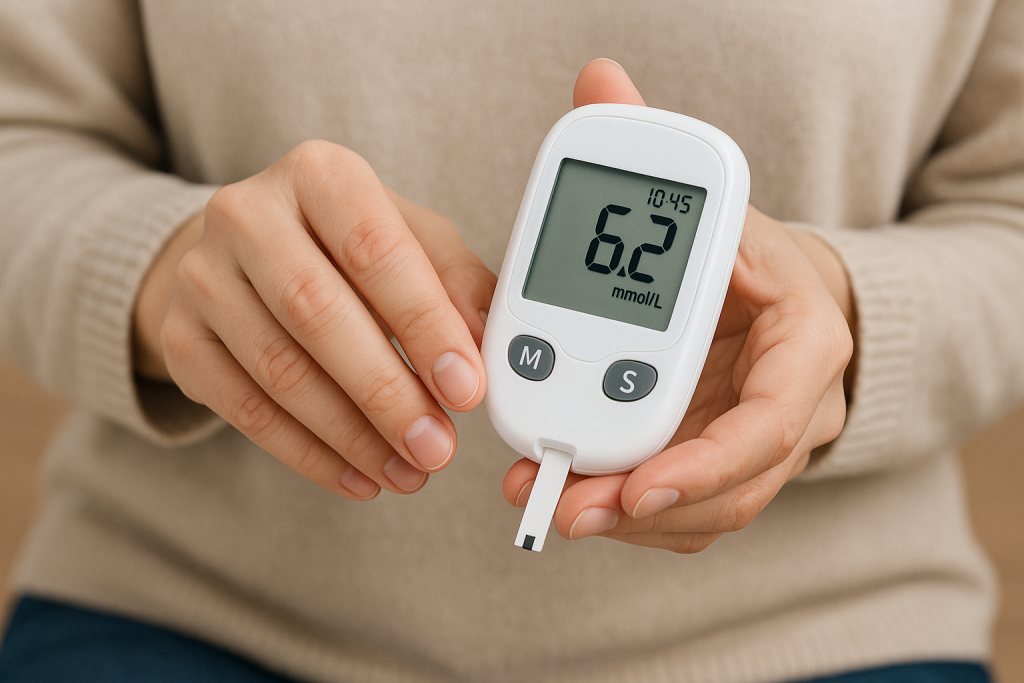
To ensure reliability, regularly calibrate your device according to the manufacturer’s recommendations. Keep your test strips away from moisture and always note the time and context (before/after meals, physical effort).
Tips and Natural Remedies to Regulate Blood Sugar
Some grandmother’s remedies rely on the power of plants and an adjusted lifestyle.
- Fenugreek: recognized for promoting insulin sensitivity. Consumed as soaked seeds or infusion.
- Cinnamon: its compounds can improve glucose uptake. Half a teaspoon per day is enough.
- Apple cider vinegar: diluted in a glass of water before meals, it slows carbohydrate digestion.
- Walking after meals: 10 minutes of light walking helps stabilize postprandial blood sugar.
“Although these practices do not replace medical treatment, they naturally integrate into a prevention routine,” emphasizes Dr. Leclerc, endocrinologist.
FAQ
What is the normal blood sugar after a meal?
Generally, the target is a level below 7.8 mmol/L (140 mg/dL) within two hours after eating. Beyond that, it is called postprandial hyperglycemia.
Should I buy a device if I am not diabetic?
Without suspicion of diabetes, a glucometer remains unnecessary. An annual blood test with your doctor is sufficient to check for any anomaly. Home tests can however be useful during a diet or an intensive sports program.
Can blood sugar be regulated without medication?
For prediabetics or those with mild insulin resistance, diet, physical activity, and natural remedies may suffice. At the slightest doubt, medical follow-up is essential.
Conclusion
Navigating between numbers and recommendations becomes more accessible when you have a complete chart, a reliable device, and some tips to temper glycemic spikes. Remember: glucose regulation is a balance between diet, exercise, and vigilance. Adjust your portions, systematically note your values, and do not hesitate to incorporate plants or spices with proven virtues.
Your blood sugar is not just a number: it is an indicator of your metabolic well-being and a guide to better habits.











