| Key Points | Details to Remember |
|---|---|
| 🧠 Definition | Diabetic neuropathy: nerve damage associated with poorly controlled diabetes |
| ⚡️ Mechanisms | Hyperglycemia damages small vessels and nerve fibers |
| ⚠️ Symptoms | Tingling, numbness, nighttime pain |
| 💊 Treatments | Medications, physical therapy, orthopedic insoles |
| 🦶 Prevention | Glycemic control, regular podiatric examinations |
| 📈 Diagnosis | Tests monofilament, electromyogram |
| 🌱 Lifestyle | Balanced diet, physical activity |
Diabetic neuropathy represents the most common nerve complication in people living with type 1 or 2 diabetes. Often noticeable only when lesions are already established, it disrupts the transmission of signals between the nervous system and target organs. However, early management can significantly reduce suffering and limit the development of irreversible sequelae.
Far from being inevitable, this nerve damage originates from poorly controlled blood sugar and a chronic inflammatory environment. And although many patients neglect it, a pathway of education, monitoring, and appropriate care greatly increases the chances of preserving sensitivity and quality of life.
Sommaire
How does neuropathy occur in diabetics?
At its core, it is the corrosive effect of sugar that weakens microcirculation. The small vessels supplying blood to nerve fibers thicken, lose their flexibility, and no longer provide enough oxygen and nutrients. At the same time, advanced glycation end products (AGEs) accumulate in tissues, disrupting neuronal functions.
Depending on the type of nerve affected, several forms are distinguished:
- Peripheral neuropathy (the most common) mainly affects the lower limbs and feet.
- Autonomic neuropathy impacts the autonomic system, responsible for cardiac, digestive, and urinary regulation.
- Proximal neuropathy, less common, causes weakness in the thigh or hip.
- Focal neuropathy manifests as paralysis of a single nerve (for example, the cranial nerve).
Each form follows its own timeline mechanism, but all share the same denominator: poorly controlled hyperglycemia.
What are the symptoms?
Sensory breakthrough in the extremities
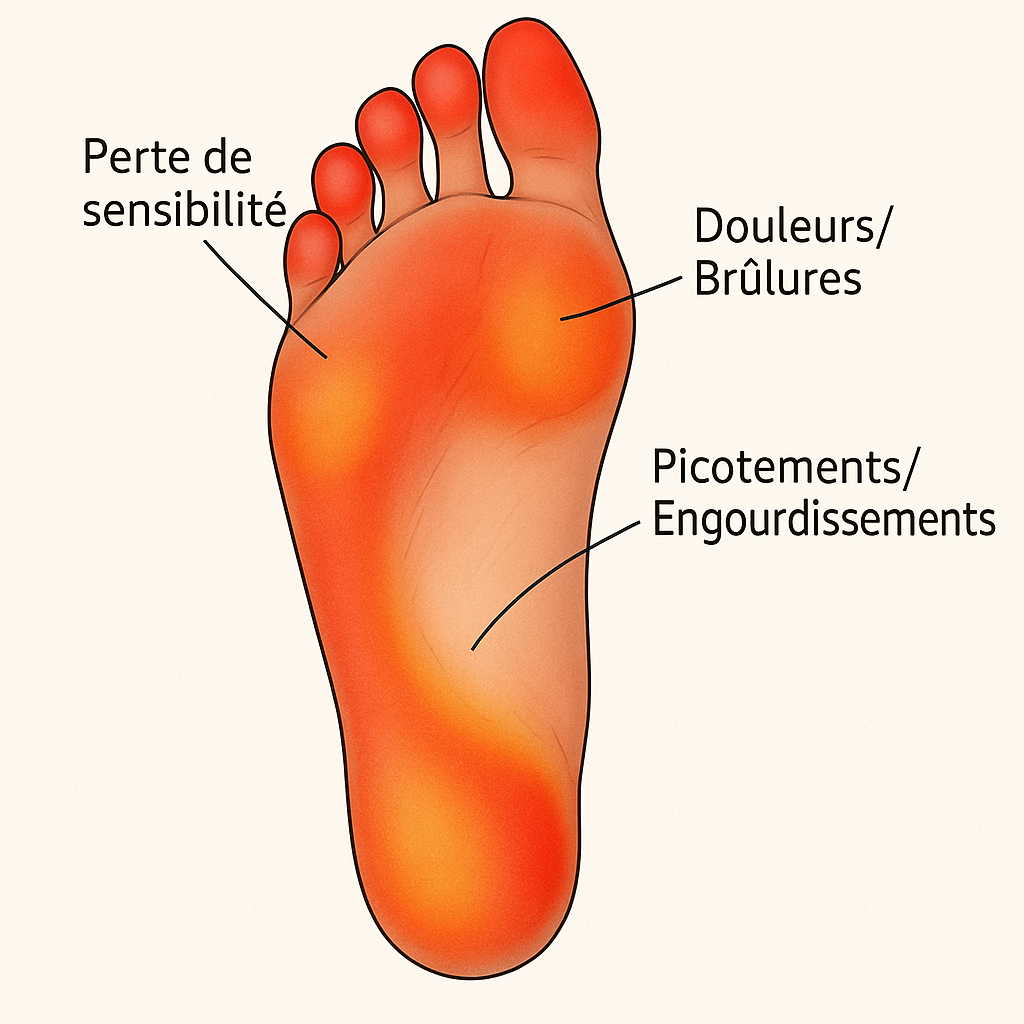
The first signals are not dramatic, often interpreted as simple fatigue or a bad sleeping position. Yet, these tingling sensations (“pins and needles”) under the soles of the feet or at the fingertips are the most common warning sign.
Over time, the sensation evolves:
- Burning sensation sometimes intense, giving the impression of walking on pebbles.
- Progressive numbness, leading to difficulty in grasping or maintaining balance.
- Nocturnal pain that disrupts sleep and forces movement without finding relief.
Motor impairment and muscle imbalance
In some cases, weakness develops. Contractility is lacking, cramps are noted, and there is an increased risk of falls. While walking, the arch of the foot may collapse, requiring custom insoles to limit the impact on the joints.
Digestive, urinary, and vascular signs
Less known, manifestations of autonomic neuropathy affect the entire body:
- Constipation or diarrhea due to slowed transit.
- Orthostatic hypotension (drop in blood pressure when standing) causing dizziness.
- Bladder disorders: urgency or incomplete emptying.
- Erectile dysfunction or vaginal dryness, often underdiagnosed.
To identify these manifestations, validated questionnaires and a targeted clinical examination will be used. Furthermore, exploring the signs of diabetes upstream quickly guides towards a thorough neurological assessment.
Possible complications: is it serious?
Without detection or intervention, loss of sensation can lead to neglect of small injuries – blisters, cuts – which become infected and deepen. Foot ulcers, increasingly common, represent the entry point to osteomyelitis.
When management is delayed, the risk of lower limb amputation rises. That is why daily monitoring (skin condition, clean socks, appropriate shoes) goes beyond a simple “routine action”: it is a vital element of the care pathway.
Diagnosis
The examination often begins with the monofilament test: a fine nylon strand applied to different areas of the foot to assess tactile perception. If the response is absent or altered, it is supplemented by:
- Nerve conduction study (electromyogram) to measure the speed of electrical transmission.
- Tendon reflexes (Achilles, patellar).
- Questionnaires such as DN4 or LANSS, validated to distinguish neuropathic pain from musculoskeletal pain.
This assessment combines clinical data and biological analyses to refine the diabetic origin and rule out other causes (vitamin B12 deficiency, hypothyroidism, alcoholism).
Available Treatments
The treatment of diabetic neuropathy is approached on two fronts: relieving pain and correcting the underlying cause.
Symptomatic Medications
Several pharmaceutical families provide real relief:
- Antineuralgics such as gabapentin or pregabalin, targeting neuronal calcium channels.
- Tricyclic antidepressants (amitriptyline) or serotonin and norepinephrine reuptake inhibitors (duloxetine).
- Capsaicin in topical cream form to locally desensitize nerve endings.
Metabolic Approach and Rehabilitation
Reducing blood sugar remains the backbone of any strategy. Intensive glycemic monitoring, combined with therapeutic education, slows the progression of lesions. At the same time, physiotherapy improves proprioception and prevents ankylosis. Custom orthopedic insoles distribute pressure, breaking the vicious cycle of pain and limping.
Supplements and Alternative Medicine
There is talk of supplements (alpha-lipoic acid, B vitamin complex), even acupuncture. These avenues deserve rigorous evaluation and never replace strict glycemic control.
Prevention and Lifestyle
Addressing the risk of neuropathy primarily relies on daily diabetes management. Here are some essential steps:
- Glycemic monitoring with a personalized goal (generally HbA1c < 7%).
- Foot examination at least once a year, more frequently if a sensitivity deficit is already present.
- Balanced diet, rich in fiber, low in fast sugars and saturated fats.
- Regular physical activity (walking, swimming, cycling) to improve microcirculation and glucose tolerance.
- Daily foot care: hydration, visual inspection, appropriate footwear (avoiding pressure points).
By synchronizing these measures, the onset of symptoms is avoided and long-term sequelae are significantly limited.
FAQ
Can diabetic neuropathy be cured?
Complete cure remains rare, as nerve fibers regenerate slowly or not at all once severely damaged. However, early diagnosis, strict glycemic control, and appropriate treatments can stop progression and reduce pain. Many patients notice a significant improvement in quality of life after a few months of care.
Does it affect all diabetics?
No, but more than 50% of people with long-standing diabetes show signs of neuropathy. The risk increases with the duration of the disease, as well as the lack of glycemic control and the presence of other complications (retinopathy, nephropathy). Active prevention reduces this incidence.
What is the difference with classic neuropathy?
The etiology here is directly linked to hyperglycemia and its metabolic consequences. In contrast, so-called “classic” neuropathy may result from nerve compression (sciatica), vitamin deficiency, or inflammatory pathology. The symptom profile and additional tests help differentiate.
When to see a neurologist?
At the first appearance of tingling or persistent numbness. The quicker the referral, the more effective the treatments will be in preserving nerve function. In case of stubborn pain or digestive/urinary disorders, collaboration between diabetologist, neurologist, and physiotherapist offers a comprehensive care pathway.
Conclusion
Diabetic neuropathy, often silent at the start, requires unwavering vigilance. Rigorous glycemic monitoring coupled with an adapted lifestyle mechanically diverts the danger. Every podiatric exam, every positive response to the monofilament, is a step towards preserving autonomy and comfort. Prevention is better than trying to cure the irreversible.
By combining therapeutic education, multidisciplinary support, and self-monitoring, it is possible to push back the limits of this complication and continue to fully enjoy life.











